Prices in Germany are normally 75% below the cost of scoliosis treatment in the US and are individually quoted. They include all medical expenses, the hospital stay, surgeon's fees, operation room fees, anesthesia, anesthesiologist's fees, medicine, nursing, semi-private room, meals, pre-op diagnosis, local phone and English TV.
Scoliosis: What is it?
Scoliosis is a condition that involves a lateral curvature of the spine; that is, the spine is bent sideways. Rotation of the spine often accompanies scolisis, adding to the complexity of the case.
There are many forms of scoliosis. The form of scoliosis determines its cause. The severity of scoliosis is measured by the Cobb angle. Scoliosis is incurable, but its natural course can be affected with treatments such as surgery or bracing.
Scoliosis: Common Variations
Common variation in scoliosis treatment are
- Anterior scoliosis surgery (Halm-Zielke Instrumentation)
- Posterior scoliosis surgery (MPDS)
- Combined anterior and posterior coliosis surgery
Scoliosis: Prevalence
Scoliosis curves greater than 10° affect 2-3% of the population, often children between the ages of ten and fourteen, with a greater incidence among girls. Curves greater than 20° affect about 1 in 2500 people. Curves convex to the right are more common than those to the left, and single or 'C' curves are slightly more common than double or 'S' curve patterns.
Different etiologic theories point to genetic, neuromuscular, hormonal and growth factors, though it appears that the cause is multifactorial. The vast majority of cases (85%) have unknown causes or are idiopathic.
In one out of every 1000 cases, surgery may be necessary. Females are nine times more likely to require treatment than males, mostly since they are also more likely to have larger, progressive curves.
Scoliosis: Symptoms
Those with scoliosis rarely complain of pain, and their condition is often discovered incidentally.
The symptoms of scoliosis are:
- Prominent shoulder blade
- Uneven hip and shoulder levels.
- Asymmetric size or location of breast in females.
- Unequal distance between arms and body
- Clothes that do not "hang right"
- Mule mass that causes a "hump" on one side of the spine
- A rib "hump"
Shoulders that have a lack of spine reinforcement can hurt if large amounts of weight are placed upon them. Back pain caused by scoliosis can manifest mainly in the younger of those affected (usually from childhood to the age of about 25) during times of heavy muscular growth, such as growth spurts, due to the irregular shaping of the spine and the resulting compensation that the person’s body has to make for that irregular shape. This pain can be anywhere from mild pain to heavier, more debilitating pain, and is often felt in the musculature directly surrounding the spine instead of in the spine itself. Due to this muscular compensation stiffness of the back and neck can also occur, especially if the curve in the spine is located higher up in the back.
Scoliosis: Associated Conditions
Scoliosis is often associated with other conditions such as neuromuscular disorders (e.g., cerebral palsy, spinal muscular atrophy, Friedreich’s ataxia); skeletal dysplasias; Marfan’s syndrome; neurofibromatosis; connective tissue disorders; and craniospinal axis disorders syringomyelia.
Scoliosis: Investigation
Those suspected of having scoliosis should undergo a thorough physical examination. During a physical examination, the following should be assessed:
- Skin for cafe au lait spots indicative of neurofibromatosis
- The feet for cavovarus deformity
- The height of the iliac crests while standing
- Magnitude of the curve and rib hump both while standing and while leaning forward
- Asymmetric shoulder and breast
- Asymmetric superficial abdominal reflexes
- Inequality of lengths of the upper limbs from the floor when leaning forward
During the exam, the patient’s gait should be assessed, and there should be a search for signs of spinal abnormalities (e.g., dysraphism as evidenced by a dimple, hairy patch, lipoma, or hemangioma). There should also be a thorough neurological examination. Ultimately, however, the main goal should be the assessment of curve severity and flexibility.
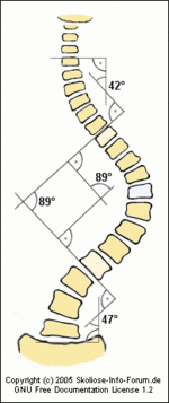
Radiograghic investigation such as X-ray or computed tomography (CT) should also be carried out to assess the location, levels of involvement, direction and magnitude of the curves. One method for assessing the curvature is the calculation of the Cobb angle, which assesses the curve from the top endplate of the topmost involved vertebra to the bottom endplate of the bottommost involved vertebra.
A note here is that most patients will be unaware that they are afflicted with scoliosis even when curves exceed 30%deg;.
Scoliosis: Management
The management of scoliosis is determined by the severity of the scoliosis and the level of skeletal maturity. A number of methods are used to decide upon the most appropriate treatment. In many instances mild scoliosis requires no treatment.
The conventional options are, in order:
- Observation
- Physiotherapy
- Bracing or casting
- Surgery
Bracing is only performed by the medical profession when the patient is in their growing years. (However, some controversial alternative treatments also advocate bracing of adults for correction; none of these have been subjected to rigorous peer reviewed study, and their efficacy is at best uncertain.) This holds the spine and prevents the curve from progressing. If a curve is maintained below 40° as the patient finishes growing, it is unlikely for it to continue progression when the brace is removed, if the curve exceeds this, surgery is often performed.
Bracing involves fitting the patient with a brace that covers the torso and in some cases it extends to the neck. The most commonly used brace is a TLSO or Boston Brace, a corset-like appliance from armpits to hips, custom-made from plastic. It is usually worn 23 hours a day and applies inward pressure on the curves in the spine. In infantile and sometimes juvenile scoliosis a body cast or plaster jacket can be used instead.
Scoliosis: Surgery
Spinal fusion is the most widely performed surgery for scoliosis. In this procedure bone (either harvested from elsewhere on the body, or donor bone) is grafted to the vertebrae so that when it heals, they will form one solid bone mass. This restricts spinal movement and prevents worsening of the curve, and straightens the curve as much as possible.
Originally spinal fusions were done without metal implants. A cast was applied after the surgery, usually under traction to pull the curve as straight as possible and then hold it there while fusion took place. Unfortunately, there was a relatively high risk of fusion failure at one or more levels (pseudarthrosis), and significant correction could not always be achieved.
The solution is metal instrumentation. This serves 2 purposes - it helps to straighten the spine, and then holds it rigid while fusion takes place. The original, now obsolete, spinal system was the Harrington rod, developed in the 1960s by Dr Paul Harrington. This long rod operated on a ratchet system, being attached by outward-facing hooks to the spine at the top and bottom of the curvature. As it was cranked out, it would distract, or straighten the curve. This system was relatively unstable in the early stages of healing, so it was still necessary to wear a cast for several months after surgery.
It also became apparent during the 1980s, as the first long term outcome data became available, that use of the Harrington for long fusions extending into the lumbar region caused problems, specifically flatback, where the loss of lumbar lordosis causes the spine to become unbalanced.
Modern spinal systems such as Luque, CD HORIZON, USS and Synergy involve a combination of rods, screws, hooks and wires fixing the spine and can apply stronger, safer forces to the spine than the Harrington rod.
>Recently types of scoliosis surgery have been trialled that aim to control a curve aggressively and delay necessary spinal fusion to allow the spine to grow to full length. These include growth rods that are extended with the spine every few months, and VEPTR or ‘titanium rib’ a metal ribcage implant, sometimes used in conjunction with a spinal implant, that pushes apart the ribs on the concave side of the curve, distracting the curve straighter without fusion. Like bracing, these are usually only effective on growing immature skeletons.
Finally, vertebral stapling is a potential alternative to fusion altogether. Staples are driven into the convex side of a curve to retard the growth of that side of the spine, allowing the other side to grow and differentially straighten the curve.
Scoliosis: Prognosis
The prognosis of scoliosis depends on the progression of the condition. Since the best outcome is the disruption or arrest of the natural history of the scoliosis, prognosis is contingent on the likelihood of progression, a factor assessed with the assignment of a Risser stage and grade. The general rules of progression are that larger curves carry a higher risk of progression than smaller curves, and that thoracic and double primary curves carry a higher risk of progression than single lumbar or thoracolumbar curves.