|
Petra Mayer (43) saddles her horse and off they go across the field. She holds the reins tight. No more problems with the right arm! |
"This was the most difficult time of my life", Petra said. "First they told me, that after 6 weeks the fracture would be healed. Unfortunately this was not the case. I still suffered pain in my right shoulder and could not use my right arm. Everything had to be done with the left arm. The normal day to day routine, such as combing hair, getting dressed and doing the housework started to become impossible. I could not drive the car or ride my horse. I was so desperate; I even had my hair cut short, as I could not groom myself. The surgeons took another x-ray and told me, that despite the metal plate no new bone tissue has been produced. I was told to go slow for another 8 weeks. In the worse case the doctors told me that they would have to operate again. Meantime my right shoulder was totally stiff from having been immobile. At this point I started to look into different alternatives as I was in two minds whether I wanted another operation due to the risks involved.

|
Four months after the accident Petra Mayer came to see our professor of orthopedic surgery, who had previously operated on her mother. Our professor is one of a few orthopedic specialists who treat difficult fractures with the new stem cell therapy. After the first check up, our professor of orthopedic surgery told Petra that she would be suitable for the stem cell therapy and the success of this operation would be very high. |
"Mrs. Mayer was suffering from a very difficult spiral fracture with lots of bone fragments.", our professor of orthopedic surgery (49) explains. Due to this, the original decision to operate was the right one. One must bear in mind, which 10% of all collar bone fractures do no heal back together." It then forms a so called "false joint". In medical terms a pseudarthrosis. The bone ends do not have the contact necessary to heal. Normally, the bone cells grow together. Instead a soft tissue forms instead of the bone connective tissue layer, which prevents further coalescence.
|
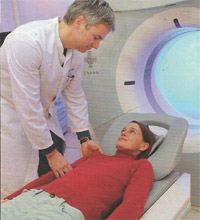
The professor states, "Soft tissue will grow instead of the bone connective tissue in between the bone endings, these will prevent a growing together of the fracture. This can happen, if for example after the first operation the screws loosen. This is not always noticeable on the X-rays, due to this we use CT images. On the CT images we can see that in case of Mrs. Mayer there was a 4 mm wide space between the bones. In cases like this, the new stem cell therapy is a successful alternative, which makes a further operation unnecessary. Petra Mayer agreed quickly to try this method. Her stem cell therapy had to be done in an operation theater for reasons of anesthesia, but it is not an operation as we would normally think of one." |
"Under a general anesthesia, the professor removed some bone marrow from my pelvic bone, isolated out of this the stem cells and injected these with a normal injection needle into the bone space of the comminuted break of my collar bone. That was all. Once I recovered from the general anesthesia, I was allowed home the same day", Petra Mayer explained.
The new therapy for bone and cartilage problems has only become possible, after scientists found how to isolate so called adult stem cells from bone marrow. As this is the body’s own tissue, there are no adverse reactions to the procedure.
The professor says, "To access the bone marrow, exactly the same method is used as would be when performing a bone marrow donation in cases of leukemia. It is obtained under sterile conditions from the pelvic bone of the patient, which we drill, using a general anesthesia, through the skin in into the pelvic bone. We remove about 60 milliliters with a syringe with a cannula. We then separate with a special centrifuge the stem cells from the blood plasma and the solid blood cells. This gives us approx. 10 milliliter of stem cell concentrate. With a syringe we injected this through Mrs. Mayer’s skin into the bone space of the comminuted break of the injured collar bone".
"In between the bone ends the stem cells will slowly change into the body’s own bone cells. The bone will grow together despite the pseudarthosis. We checked Mrs Mayer’s improvement every 4 weeks with CT scans. The 4 mm wide space was down to 2 mm within one month. 2 months later the space was 1 mm and after 3 months it had totally closed. Since then the collar bone has been stabile and is fully resilient."
After the treatment Mrs. Mayer improved daily. "Soon the pain had disappeared. After physiotherapy I was able to fully use the arm again. The muscles, which had become weak over the long immobilization, were starting to gain strength again."
To date, the professor has already helped around 100 patients successfully with this stem cell therapy method. Next to poorly healing breaks, such as a comminuted break, this method is also used for arthritis and other cartilage damage, tendon injuries and dying bone tissue, for example in the hip joint.
Petra Mayer said it was more than worth it, "Most of all I am so happy that I can ride my horse again. I do not blame my horse for throwing me off; as I am aware he did not mean to harm me. The modern stem cell therapy has given me a new lease on life. Only after being injured for a long time, one appreciates the importance of being healthy and being able to move normally."
|
|
|
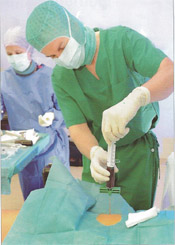
Step One: The Professor removes approximately 60 ml of bone marrow from the iliac crest.
Step Two: The bone marrow is injected into the container.
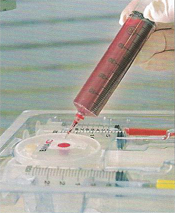
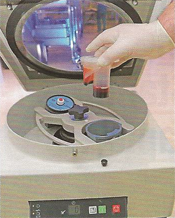
Step Three: The fluid is placed in the centrifuge and spun for 15 minutes.
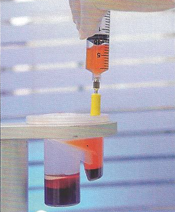
Step Four: The layer of blood plasma is removed.
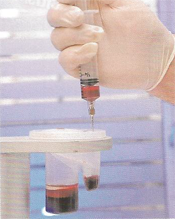
Step Five: The layer of stem cells is captured.
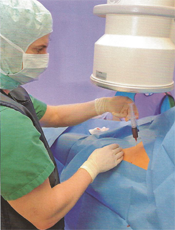
Step Six: The stem cells are injected under fluoroscopic guidance.
|
|
|